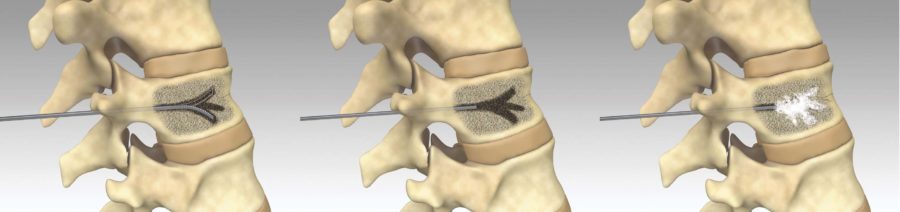
Treatments for Vertebral Fractures
Treatment for vertebral fractures depends on how recent the fracture is, the duration of discomfort, the type of fracture and the degree of disability.
Options for short-term treatment include pain control and physical therapy. Long-term emphasis is on treating underlying conditions such as osteoporosis.
In cases of pain that is not well controlled despite medication, severe debilitation, or in patients who cannot receive or tolerate pain medications, vertebral augmentation may be indicated. Vertebral augmentation includes treatments like Vertebroplasty and Kyphoplasty.
Your Interventional Radiologist in conjunction with your primary care doctor will assist in guiding you through the appropriate route of management.